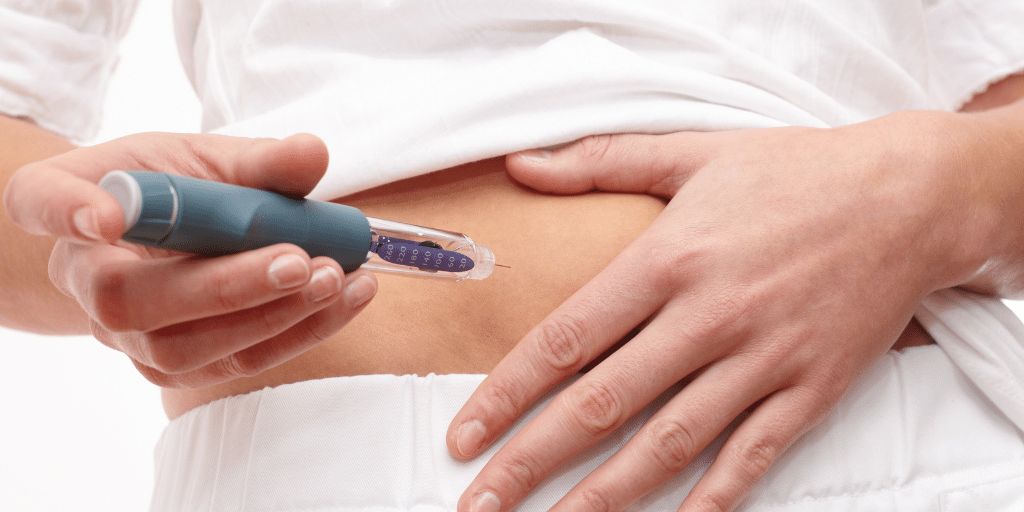
Ozempic, Wegovy, Mounjaro, and Zepbound are trending big time right now. You likely know someone who has seemingly shrunk overnight and found out they took this “magic” drug. Or maybe you watched an influencer inject themselves on TikTok and go from a size 20 to 12 in months. Originally developed for type 2 diabetes, these drugs are also popular with socialites and celebs like Chelsea Handler, Khloe Kardashian, and Elon Musk. If you have PCOS and are struggling with your weight or other metabolic issues, you may be wondering if Ozempic, Wegovy, Mounjaro, or Zepbound are right for you. Read on to learn more about these medications for PCOS, including the pros and cons.
*updated 8.21.24
PCOS And Metabolic Phenotype
In order to understand if these medications could be helpful for PCOS, it’s important to first understand the different PCOS phenotypes – as PCOS is not a one-size-fits-all condition. The most common phenotype is called phenotype A or classic PCOS. This type has higher rates of metabolic disorders, including risk of diabetes and cardiovascular heart disease. Signs and symptoms can include obesity, visceral abdominal fat, hypertension, greater insulin resistance, fatty liver, elevated lipids, and elevated blood sugar. Up to 70% of PCOS patients are obese, and 50-90% of PCOS patients have insulin resistance. Further, as per the CDC, 50% of PCOS patients get prediabetes or diabetes by age 40.
Weight loss decreases health risks in the metabolic phenotype. The international evidence-based guideline for the assessment of PCOS recognizes the importance of weight reduction to help promote better metabolic, reproductive, and cardiovascular outcomes in PCOS patients who are overweight or obese. But this is easier said than done! Many PCOS patients face multiple hurdles to losing weight, such as insulin resistance (which can promote more fat storage, cravings, and constant hunger), altered hunger hormones, negative body image, depression, and fatigue, which can make exercise more difficult.
In addition, treatment for PCOS tends to be overly weight-focused – which can backfire. Patients are often told to eat less, cut out all carbs, and exercise more, without even asking what their current diet or exercise routine is like. Patients may be accused of eating too much if the scale doesn’t go down – and basically fat-shamed. This only compounds the patient’s frustrations with trying to lose weight and exacerbates the risk of eating disorders. To make it even more complicated, there are higher rates of eating disorders in PCOS, so it can be a slippery slope.
The dilemma is that weight loss can help decrease health risks for PCOS patients’ metabolic phenotype, yet many PCOS patients experience difficulty losing weight. So it’s only natural that you might be curious about these new medications—so let’s dive in!
The Basics On Ozempic, Wegovy, Mounjaro And Zepbound
Ozempic and Wegovy belong to a class of drugs called incretin mimetics. They mimic natural gut hormones that can lead to decreases in blood sugar, body weight, cholesterol, and blood pressure. Incretin mimetics were developed in the early 2000’s after researchers noticed poisonous lizards known as Gila monsters have a unique ability to maintain steady blood sugar levels even after long stretches of not eating. Venom from this lizard inspired the development of exenatide (Byetta), the first in this class of drugs.

Ozempic
Ozempic was approved by the FDA in 2017 to treat type 2 diabetes. In addition to lowering blood sugar, it helps people with diabetes lower their risk for cardiovascular events like heart attack or stroke by 24% compared to placebo. Reference: SUSTAIN 6 and PIONEER 6 trials. It comes in three doses: 0.5, 1.0, and 2.0 milligrams given in a once-a-week injection. There is also a pill form of semaglutide called Rybelsus.
Wegovy
Wegovy is the exact same drug as Ozempic but at a higher dose. It was approved by the FDA in June 2021 to treat chronic weight management in patients with a body mass index (BMI) of 27 or greater who have at least one weight-related ailment or in patients with a BMI of 30 or greater, regardless of weight-related ailments. Wegovy can start at .25 mg/0.5 mL and be dosed up to 2.4 milligrams per week.
Note: people without type 2 diabetes have begun using Ozempic off-label for weight loss due to a shortage of Wegovy, partly brought on by the Ozempic’s weight loss effects going viral on social media. This is a problem for people with diabetes … as they often have trouble getting access to the drug! This shortage is also a problem for those with obesity who also benefit from Wegovy.
Mounjaro
Tirzepatide, brand name Mounjaro, is a newer drug that is also gaining in popularity. It’s the first medication that mimics two hormones found in the body – GIP (glucose-dependent insulinotropic polypeptide) and GLP-1. It is approved for type 2 diabetes. The SURMOUNT-1 study showed that study participants who did not have diabetes taking tirzepatide lost up to 22.5 percent of their body weight after 72 weeks.
Zepbound
The brand name drug, Zepbound, is the same as Mounjaro. It was fast-tracked by the FDA and approved in 2023 for adults who are obese or overweight. Dosing for Zepbound is the same as Mounjaro, and it works in the exact same way. The only difference is that it’s rebranded for the purpose of weight loss rather than type 2 diabetes. Zepbound starts at 2.5 mg dosing and incrementally increases to achieve a therapeutic dose of 15 mg with weekly injections.
Further research has shown that medications with tirzepatide (Zepbound and Mounjaro) show nearly a 7% greater reduction in weight after 12-months in overweight and obese patients when compared to Ozempic or Wegovy. Side effects reported were relatively similar between patients taking either drug, however the GI side effects on average were more tolerable with tirzepatide.
There is an even newer drug on the block in clinical trials that is looking to produce even greater weight loss results in an even shorter period of time than the drugs mentioned above. Stay tuned for an update to this blog post once we have more news on the FDA approvals. The drug is showing potential in clinical trials to produce an average loss of 24% total body weight in patients after one year on the medication, potentially setting a new milestone in the weight loss medication space.
Effects on Blood Sugar and Weight

- Lowering blood sugar
When we eat, our gut produces a hormone called glucagon-like peptide 1. This tells our body to release insulin to help lower blood sugar. It also reduces the release of glucagon—a hormone that increases blood glucose—thereby also helping to control blood sugar. Semaglutide (Ozempic & Wegovy) works by activating GLP-1 receptors throughout the body and enhancing the effects of the naturally occurring hormone GLP-1 – with the effects noted above. One study showed that 1 mg of Ozempic can lower HbA1c from 8.7 to 6.7 in 16 weeks. As a certified diabetes care and education specialist, I find this to be very impressive!

- Promoting weight loss
In addition to lowering blood sugar, semaglutide can help with weight loss. In one large double-blind trial clinical trial, 1,961 adults with excess weight or obesity who did not have diabetes were given 2.4 milligrams of semaglutide or a placebo once a week for 68 weeks, along with lifestyle intervention. Those who took semaglutide lost 14.9% of their body weight compared with 2.4% for those who took the placebo. While we don’t know the exact mechanisms, semaglutide appears to:
-Affect the hunger center in the brain, specifically the hypothalamus. This reduces cravings, appetite, and hunger.
-Slows the rate of stomach emptying, which prolongs fullness and satiety after meals. This means you aren’t as hungry and end up eating less. Many people also say it just takes away their interest in (or sometimes obsession with) food. Basically, this drug works by helping you to eat less – not by “speeding up your metabolism”.
Does The Weight Loss Eventually Stop?
Based on data from the SUSTAIN FORTE trial, we know that weight loss peaks by one year and is maintained during the second year on the drug. However, the study ended then, so we don’t know what happens after two years. Read below to see 
The hardest part of weight loss isn’t losing the weight, it’s keeping it off. One of the biggest concerns with these drugs is the weight regain once you stop them. A study showed that weight regain happens as soon as you stop the drug. After one year of being off the drug, here is what’s projected to happen if you had lost:
– < 5% of your body weight, you will gain more weight than what you started at
– 10-15% of your body weight, you’ll probably end up at the weight you started at
– 20% or more of your body weight, you’ll likely keep off 1/3 of the weight you lost
Another recent and large study of over 20,000 patients from EPIC showed that over half of patients taking semaglutide and another GLP-1 agonist called liraglutide were able to maintain their lower weight for a year or longer after no longer using the medication. They noted that about 17% of patients that were on semaglutide in this study gained back all the weight they lost from the medication or more.
Will you gain back ALL the weight in the next year? We just don’t know. Still, as expected, as soon as the drug was stopped, blood glucose, blood pressure, and blood lipids went back up. This reinforces the fact that these medications are meant for chronic use.
I often get asked if you stop the drug, but continue the healthy diet, exercise, and other lifestyle habits, can you keep the weight off? The above study did not take any of this into account. My guess is that at least some of the weight would be regained. However, I have read comments on social media where people said they lost weight (sometimes a lot) on these meds and have kept it off by being very diligent with diet and exercise. Since these meds cut the appetite tremendously, you would have to consume the same amount of calories once off the med that you were consuming while taking the medication to have a chance of keeping the weight off. However, I don’t have any “studies” to corroborate this.
In my opinion, if someone had been lean much of their life then experienced a weight gain for a specific reason (i.e. broke their leg and couldn’t exercise), they would have a greater chance of keeping the weight off once they came off the drug as compared to someone who had been overweight much of their life.
Pros And Cons Of Ozempic, Wegovy, Mounjaro And Zepbound For PCOS
You may think these medications sound magical, but as with any medication, there are pros and cons, as well as potential side effects. That’s why it’s important to discuss these with your doctor in depth. I would also recommend working with a doctor trained in obesity medicine—or at least one with extensive experience prescribing these medications.
Pros
- Promotes weight loss by decreasing appetite and promoting satiety, which leads to a decrease in caloric intake. They slow down the rate at which food is emptied from the stomach, which keeps you feeling full longer.
- Lowers blood sugar.
- May also lower cholesterol levels by reducing the production of LDL (low-density lipoprotein) cholesterol and increasing the production of HDL (high-density lipoprotein) cholesterol.
- Reducing inflammation. PCOS is associated with low grade inflammation. GLP-1 medications may reduce inflammation by inhibiting the activity of pro-inflammatory cytokines, which are molecules that promote inflammation in the body.
- Lowers blood pressure.
- Can take away constant thinking about food or “food noise”
- Decreases risk of heart disease for those with diabetes.
Cons
- Need to be on them long term – but keep in mind that many other meds are needed long term for chronic health conditions, like drugs for thyroid disorders or high blood pressure.
- Weight will likely be regained once stopping them
- Shortages often occur
- Can be expensive if not covered by insurance. If prescribed off label, it’s highly unlikely your insurance company will pay for semaglutide. For example, if you are obese and are trying to get a prescription for Ozempic, but don’t have diabetes (and there is a Wegovy shortage), you may have to pay $1500/month! Talk to your doctor or pharmacist to find ways to lessen the cost (such as with coupons). But keep in mind things can change with these coupon programs or even with your insurance, so you may be left without the medication.

- Serious side effects can include (taken from drug website): thyroid tumors, including cancer, pancreatitis, kidney problem, vision changes, gall bladder problems. Please read the Ozempic /Wegovy and Mounjaro/Zepbound website for more detailed information and talk with your doctor if this medication is right for you. They are contraindicated if you have certain medical conditions.
- Malnutrition: there are some reports of patients experiencing malnutrition where their bodies aren’t receiving adequate nutrients, including protein. This can have a negative effect on overall health.
- Loss of muscle mass: Whenever you lose a significant amount of weight, you lose fat and muscle – the average being 20-30% loss from lean mass. As per Dr. Spencer Nadolslky, obesity and lipid specialist physician and medical director of Sequence, studies on semaglutide showed patients lost 38% loss of lean mass and low to mid 20% loss of lean mass from tirzepatide. But he says he has over 24,000 patients in his obesity medicine program and has not seen anything over a 20% loss of lean mass from DEXA scans. We need more studies on this! Consuming adequate protein and weight training can help to slow this loss.
Is Ozempic, Wegovy, Mounjaro Or Zepbound Helpful For PCOS?
My answer is … it depends on many factors.
But first, I want to let you know that you can still be overweight and be healthy if you have PCOS. It’s also possible to lose weight if you have PCOS without weight loss medications. Over the past 20 years, I’ve helped thousands of PCOS patients improve their symptoms and decrease health risks. We work on habits, nutrition, meal timing, mindset, sleep, stress, and add in targeted supplementation. Many of those patients also lose a significant amount of weight as well. So, most people do not need these weight loss drugs. But some patients are doing everything “right” and the scale barely budges, and they still have the metabolic risk factors. These are the patients for whom these medications might be appropriate!
If you are considering semaglutide, here are a few factors to keep in mind to see if they could be right for you:
Meet the criteria for these drugs
These medications are not for people who want to lose 10 pounds! As per the FDA, the criteria for these medications are a body mass index (BMI) of 27 or greater who have at least one weight-related ailment (which many PCOS patients have) or patients with a BMI of 30 or greater. Perhaps the criteria will change as more studies are done with PCOS patients.
Metabolic PCOS phenotype
This was discussed in the first section. The metabolic phenotype has higher rates of metabolic disorders, including risk of diabetes and cardiovascular heart disease. Signs and symptoms can include obesity, visceral abdominal fat, hypertension, greater insulin resistance, fatty liver, elevated lipids, and elevated blood sugar. Weight loss improves health risks associated with the metabolic phenotype of PCOS.

Too often, I’ve heard patients tell me their doctor prescribed one of these medications without recommending they work with a nutritionist first or getting a detailed history of their past dieting attempts. Managing PCOS should always start with diet and lifestyle. Work with a nutritionist who specializes in PCOS first to learn good habits. When you’ve worked with a nutritionist and find you just can’t lose weight on your own, and you and your doctor feel weight loss would benefit your PCOS, then you could consider these medications.
Understand that they are long-term medications
Obesity is a chronic condition. Studies have shown most (or all) of the weight loss that occurs while on these drugs is regained within a year. In addition, a good percentage of the weight you lose is from muscle, especially if you don’t weight train and consume adequate protein. Then, when you regain the weight, much of it comes from fat, so you end up with a higher body fat percentage.
Approximately 30% of PCOS patients have elevated levels of adrenal androgens, which worsen PCOS symptoms. Eating too few calories and rapid weight loss can act as a stressor, possibly increasing adrenal androgens. We need more studies on this.
You do not have a history of an eating disorder
For some people, these medications may improve their relationship with food by cutting out the “food noise” in their heads. But for others, the lack of appetite may cause you to skip meals, possibly bringing up old eating disorder issues or causing new ones. I strongly discourage people from taking these meds with any form of disordered eating.
My Opinion

There are no FDA-approved medications for treating PCOS. All the common meds used, such as BCP, metformin, and spironolactone, are prescribed off-label. While it’s ideal to treat PCOS naturally with nutrition, lifestyle, and targeted supplementation, sometimes symptoms and health risks cannot be managed naturally. It would be great to have another tool such as semaglutide/tirzepatide medications in our toolbox to help manage PCOS for certain patients.
But keep in mind these are not magic pills. They do not cure PCOS or fix all the hormone imbalances associated with PCOS. For example, you could still have elevated DHEAS from the adrenal glands, dysregulated cortisol patterns, and thyroid imbalances, to name a few. We don’t know how these medications affect the HPA/HPO axis. In addition, some people are unable to tolerate the side effects.
Tips For Taking Ozempic, Wegovy, Mounjaro Or Zepbound
If you decide on of these medications may be right for you, keep these tips in mind:

- Focus on nutrient-rich foods. Food quality plays a crucial role in improving PCOS symptoms, improving fertility and decreasing health risks. You may find your appetite is greatly reduced, but make sure you focus anti-inflammatory foods rich in vitamins, minerals, fiber and phytochemicals.
- Consume adequate protein to help slow loss of muscle mass. Dr. Spencer Nadolsky recommends 1 – 1.2 gm protein per kg of body weight (divide weight in pounds by 2.2 to get kg). This would be 113-136 gm of protein if you weighed 250 pounds. Protein shakes or protein powder can be an easy way to bump up protein if your intake is low. It’s also a good idea to consume “chunks” of protein throughout the day versus eating minimal protein during the day and loading up at dinner. Your body utilizes protein better this way.
- Make exercise a priority. As mentioned previously, any time you lose weight, you also lose muscle. Large weight losses can mean more muscle loss. Weight training is the most important type of exercise to help slow the loss of muscle mass. I’d recommend weight training 3x/wk. This also helps to keep your metabolism moving. In addition, aerobic exercise is important for heart health.
- If possible, get a DEXA scan to track changes in lean mass while on the medication.
- Consume adequate fluids to stay hydrated. These meds may take away your thirst as well. Water and tea are my favorite beverages for PCOS.
- Find ways to manage stress. PCOS is a hormonal imbalance, and stress can wreak havoc on your whole body, including thyroid, adrenal glands (which can lead to more androgen production), reproductive health, and more.
- Mood issues can still be there. Weight loss may help improve self-esteem and some mood disorders, but it doesn’t necessarily take away clinical depression/anxiety. Seek help if needed.
- Start with the lowest dose and taper up slowly. This can help decrease side effects.

- Don’t compare your journey to others. Everyone loses weight at a different rate.
- Unfollow/unfriend those social media accounts that cause you anxiety about taking these meds or weight in general
- If you decide to try to stop using it, make sure you have a great diet, exercise, sleep, and stress management program in place.
- Beware when TTC. These drugs are not approved for use during pregnancy. Most doctors recommend stopping them for 2 months before getting pregnant. Use effective contraception while taking these medications.
- Be confident that your insurance will cover the medication (or you have the funds to pay out of pocket). It would not be good mentally or physically to lose a large amount of weight, only to regain it.
- If you decide to take one of these medications, don’t let anyone shame you! Just like fat shaming is horrible, so is shaming people for wanting to lose weight, actually losing weight, or losing weight with the assistance of a medication. Obesity is a chronic disease. Just like you take medications for high blood pressure, some people can really benefit from medications for weight.
- If you are on the fence about these medications, don’t feel pressure to start them right now. These medications aren’t going anywhere, and more incretin mimetic drugs are currently being developed. By waiting a bit longer before jumping on the bandwagon, we’ll have more long-term studies and more studies done with PCOS.
I’d love to hear your thoughts on these medications. Have you tried one of them?
References:
Efficacy and safety of once-weekly semaglutide 2·0 mg versus 1·0 mg in patients with type 2 diabetes (SUSTAIN FORTE): a double-blind, randomised, phase 3B trial
DOI: 10.1016/S2213-8587(21)00174-1
SUSTAIN 6 and PIONEER 6 trials
Figures in article taken from https://www.nejm.org/doi/full/10.1056/NEJMoa2107519
https://www.sciencedirect.com/science/article/pii/S2667368122000079
https://www.nejm.org/doi/full/10.1056/NEJMoa2032183